Eliza Brader worries she quickly might want to show she’s working to proceed receiving Medicaid well being protection. She doesn’t suppose she ought to need to.
The 27-year-old resident of Bloomington, Indiana, has a pacemaker and a painful joint illness. She additionally has fused vertebrae in her neck from a spinal damage, stopping her from turning her head.
Indiana’s Medicaid company at present considers Brader “medically frail,” giving her entry to an expanded set of advantages, comparable to bodily remedy.
New federal guidelines would require greater than 18 million Medicaid enrollees nationwide to indicate they’re working, volunteering, or going to high school for 80 hours a month beginning in 2027 to maintain their protection. Brader is exempt so long as she’s deemed medically frail.
However missing enough federal steering, states are wrestling with outline medical frailty — a consequential resolution that would reduce Medicaid protection for many individuals, mentioned state officers, client advocates, and well being coverage researchers.
“It’s terrifying,” Brader mentioned. “I have already got fought so laborious to get my well being care.”
‘Extremely Excessive’ Stakes
President Donald Trump’s One Large Lovely Invoice Act slashes almost $1 trillion from Medicaid over the subsequent decade, with a lot of the financial savings projected to return from now not protecting those that don’t qualify below the brand new work guidelines. These spending cuts assist offset the prices of GOP priorities, comparable to additional border safety and tax cuts that primarily profit the rich.
Conservative lawmakers have argued that Medicaid, the federal government medical health insurance program for individuals with low incomes or with disabilities, has grown too giant and costly, particularly within the wake of its growth to extra low-income adults below the Inexpensive Care Act. In addition they say that requiring individuals to work is widespread sense.
The work guidelines in Trump’s tax-and-spending legislation supply exemptions for a number of teams who may battle to fulfill them, together with individuals deemed “medically frail.” The legislation spells out sure “medically frail” circumstances comparable to blindness, incapacity, and substance use dysfunction. Nevertheless it doesn’t checklist many others.
As an alternative, the legislation exempts these with a “critical or complicated medical situation,” a time period whose interpretation might differ by state.
State officers say they want extra readability to make sure that individuals who can not work for well being causes retain rightful entry to Medicaid. In addition they fear that, even with a transparent definition, individuals will face the onerous process of getting to recurrently vouch for being medically frail, which is a problem with out dependable entry to medical care.
“The stakes are extremely excessive,” mentioned Kinda Serafi, a companion at consulting agency Manatt Well being.
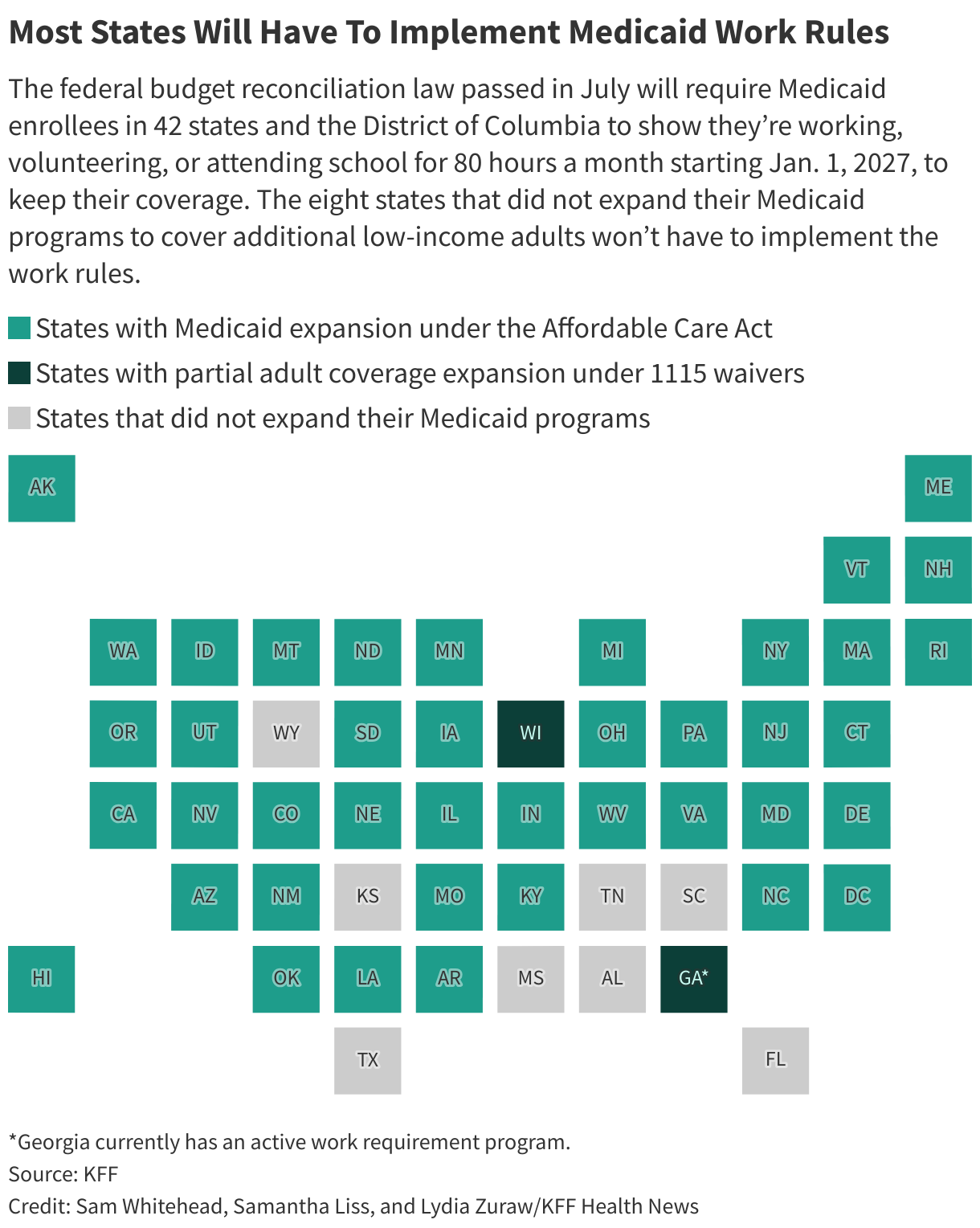
The brand new work necessities will have an effect on Medicaid recipients in 42 states and Washington, D.C. Eight states — Alabama, Florida, Kansas, Mississippi, South Carolina, Tennessee, Texas, and Wyoming — didn’t develop their Medicaid applications to cowl further low-income adults, in order that they gained’t need to implement the work guidelines.
The Medicaid work guidelines are anticipated to be the largest driver of medical health insurance protection losses over the subsequent decade, in keeping with the nonpartisan Congressional Funds Workplace.
Forty-four % of all adults coated by states’ expanded Medicaid applications have not less than one continual well being situationin keeping with KFF.
A Problem for States
State Medicaid companies are scrambling to implement the foundations with little path from the U.S. Division of Well being and Human Companies, which has but to challenge particular steering. Federal officers will make clear the “medically frail” definition subsequent 12 months, mentioned Andrew Nixon, an company spokesperson.
Finally, states must resolve who’s unhealthy sufficient to be exempt from work guidelines. And it gained’t be straightforward for state staff and their pc techniques to trace.
Yearly, state eligibility techniques display hundreds of thousands of candidates to verify in the event that they qualify for Medicaid and different authorities applications. Now, these identical techniques should display candidates and present enrollees to find out whether or not they meet the brand new work guidelines.
Jessica Kahn, a companion at consulting agency McKinsey & Co., has urged states to begin planning adapt eligibility techniques to confirm work standing. States can do a “large quantity” of labor with out path from the federal authorities, mentioned Kahn, a former federal Medicaid techniques official, who spoke throughout a latest Medicaid advisory panel listening to. “Time is a-wasting already.”
State Medicaid administrators are pondering the problem.
“Medical frailty will get so complicated,” Emma Sandoe, Oregon’s Medicaid director, mentioned throughout a latest panel dialogue. Circumstances that may maintain individuals from working, comparable to psychological well being issues, could be laborious to show, she mentioned.
A state may attempt to use knowledge pulled from an individual’s well being information, as an illustration, to find out medical frailty. However info from a affected person’s chart might not paint a transparent image of somebody’s well being, particularly in the event that they lack common entry to medical care.
It’s a tall order for eligibility techniques that traditionally haven’t needed to scrape medical information to display candidates, mentioned Serafi of Manatt Well being.
“That’s an extremely new factor that eligibility enrollment techniques are simply not fluent in in any respect,” Serafi mentioned.
Lobbying teams for the non-public medical health insurance firms that assist run Medicaid in lots of states even have urged federal regulators to obviously outline medical frailty so it may be utilized uniformly.
In a Nov. 3 letter to federal officers, the Medicaid Well being Plans of America and the Affiliation for Group Affiliated Plans advocated for permitting enrollees to qualify for the exemption by saying on their purposes that they’ve circumstances that make them medically frail. Efficiently implementing exemptions for the medically frail will likely be “essential” given the “extreme well being dangers of protection loss for these populations,” the teams mentioned.
Some state officers fear about unintended penalties of the work guidelines for individuals with continual circumstances.

Jennifer Strohecker, who not too long ago resigned as Utah’s Medicaid director, reiterated the excessive stakes, particularly for these with diabetes on Medicaid. They could be very wholesome and practical with insulin, but when they fail to finish the work necessities, which will change, Strohecker mentioned throughout a latest Medicaid advisory listening to.
Whether or not somebody is deemed medically frail already relies upon closely on the place they stay.
For instance, in Arkansas, individuals point out on their Medicaid purposes that they’re disabled, blind, or need assistance with each day dwelling actions.
Roughly 6% of the roughly 221,000 individuals enrolled in Arkansas’ Medicaid growth program are deemed medically frail, in keeping with Gavin Lesnick, a spokesperson for the Arkansas Division of Human Companies.
In West Virginia, the state accepts a medical frailty designation when an applicant self-reports it.
The burden of proof is increased in North Dakota. Candidates there should reply a questionnaire about their well being and submit further documentation, which can embrace medical chart notes and remedy plans. Greater than half of candidates have been denied final 12 months, in keeping with Well being and Human Companies Division spokesperson Mindy Michaels.
Indiana’s Household and Social Companies Administration, which runs its Medicaid program, declined an interview and mentioned it couldn’t touch upon particular person circumstances, like Brader’s.
Brader worries the extra crimson tape will trigger her to lose Medicaid once more. She mentioned she was quickly kicked off this system in 2019 for failing to fulfill the state’s work guidelines when Indiana mentioned her work-study job didn’t depend as employment.
“Anytime I’ve tried to obtain assist from the state of Indiana, it has been a bureaucratic nightmare,” she mentioned.
As states await federal steering, Kristi Putnam, a senior fellow on the conservative Cicero Institute and former secretary of the Arkansas Division of Human Companies, which oversees the state Medicaid program, mentioned even when a state creates an intensive checklist of qualifying “medically frail” circumstances, the road should be drawn someplace.
“You possibly can’t probably create a coverage for exemptions that may catch every part,” she mentioned.